Understanding Kidney Disease
Kidney disease, also known as renal disease, refers to conditions that impair the kidneys’ ability to filter waste products, toxins, and excess fluid from the blood. The kidneys play a critical role in maintaining overall health by regulating electrolytes, blood pressure, fluid balance, and hormone production.
Healthy kidneys filter approximately 150–180 liters of blood per day, removing metabolic waste products and maintaining proper chemical balance within the body. When kidney function declines, toxins and excess fluids can accumulate, potentially leading to a range of health complications.
Kidney disease may develop gradually over time or occur suddenly due to injury or illness. Early stages often produce few symptoms, which is why the condition may progress silently until kidney function becomes significantly impaired.
In addition to conventional medical management, regenerative medicine therapies including stem cells, exosomes, platelet-rich plasma (PRP), and platelet-rich fibrin (PRF) are being studied for their potential role in supporting cellular repair, reducing inflammation, and promoting tissue regeneration within damaged kidney tissue.
Types of Kidney Disease
Kidney disease includes a variety of conditions that affect kidney structure and function.
Chronic Kidney Disease (CKD)
Chronic kidney disease is the gradual loss of kidney function over months or years. It is one of the most common kidney conditions worldwide.
CKD is typically classified into five stages based on the kidneys’ filtering ability, known as the glomerular filtration rate (GFR).
Contact Us
Common causes include:
- Diabetes
- High blood pressure
- Chronic inflammation
- Autoimmune disorders
- Genetic kidney conditions
If left untreated, CKD may eventually progress to kidney failure, requiring dialysis or kidney transplantation.
Acute Kidney Injury (AKI)
Acute kidney injury is a sudden decline in kidney function that occurs over hours or days. AKI may result from:
- Severe infection
- Reduced blood flow to the kidneys
- Toxic medication exposure
- Major surgery
- Trauma
In many cases, kidney function can improve if the underlying cause is treated promptly.
Polycystic Kidney Disease
Polycystic kidney disease (PKD) is a genetic disorder characterized by the development of fluid-filled cysts within the kidneys.
Over time, these cysts can enlarge and disrupt normal kidney function.
Glomerulonephritis
Glomerulonephritis is an inflammatory condition affecting the glomeruli, the microscopic filtering units within the kidneys.
Inflammation in these structures can impair the kidney’s ability to filter blood effectively.
Diabetic Kidney Disease
Long-term high blood sugar levels associated with diabetes can damage the delicate blood vessels in the kidneys, leading to diabetic nephropathy, one of the most common causes of chronic kidney disease.
Symptoms of Kidney Disease
Early stages of kidney disease may produce few noticeable symptoms. As kidney function declines, symptoms may include:
- Fatigue
- Swelling in the legs or ankles
- Changes in urination
- Shortness of breath
- Nausea or vomiting
- Muscle cramps
- Difficulty concentrating
- High blood pressure
These symptoms occur as waste products and fluid accumulate in the body.
The Role of Inflammation and Cellular Damage
Chronic kidney disease often involves persistent inflammation, oxidative stress, and progressive tissue damage.
Damage to the kidneys can affect several key structures including:
- Glomeruli (filtering units)
- Tubules (reabsorption channels)
- Interstitial tissue
- Blood vessels
Inflammation can lead to fibrosis, a process in which normal kidney tissue is replaced with scar tissue. This scarring reduces the kidneys’ ability to filter blood effectively.
Because kidney tissue has limited regenerative capacity, preventing further damage and supporting tissue repair are important goals in kidney disease management.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative Medicine and Kidney Health
Regenerative medicine focuses on supporting the body’s natural healing processes through biologically active therapies that may promote cellular repair, anti-inflammatory signaling, and tissue regeneration.
Emerging research is exploring how therapies such as stem cells, exosomes, PRP, and PRF may support kidney function by influencing cellular communication and promoting regenerative processes.
These therapies are being investigated for their ability to help address underlying biological mechanisms associated with kidney injury.
Stem Cell Therapy for Kidney Disease
Stem cells are specialized cells capable of differentiating into multiple cell types and releasing signaling molecules that support tissue repair.
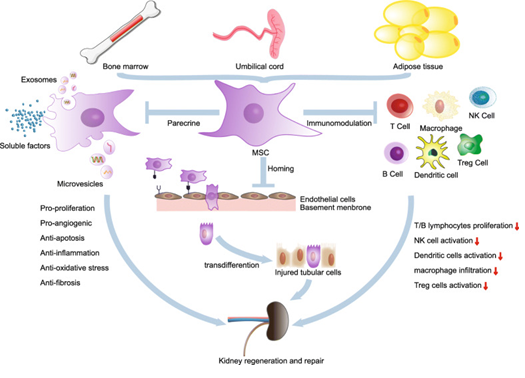
In kidney research, mesenchymal stem cells (MSCs) are of particular interest due to their regenerative and anti-inflammatory properties.
Potential mechanisms being studied include:
- Reducing inflammatory signaling in kidney tissue
- Supporting regeneration of damaged kidney cells
- Promoting blood vessel repair within the kidneys
- Reducing fibrosis and scar formation
- Improving cellular communication during tissue repair
Researchers are investigating stem cell therapies for a variety of kidney conditions including chronic kidney disease and acute kidney injury.
Exosome Therapy
Exosomes are microscopic extracellular vesicles released by cells that function as biological communication signals.
They contain proteins, lipids, and RNA molecules that help regulate cellular behavior and tissue repair.
In kidney disease research, exosomes are being studied for their potential ability to:
- Support regeneration of kidney cells
- Reduce inflammation in kidney tissue
- Improve communication between repair cells
- Promote vascular repair within the kidneys
- Improve mitochondrial function in stressed cells
Because exosomes deliver signaling molecules rather than whole cells, they are being investigated as a potential way to deliver regenerative signals to damaged organs.
Platelet-Rich Plasma (PRP)
PRP is produced from a small sample of the patient’s own blood and contains concentrated platelets that release growth factors involved in tissue repair.
Important growth factors found in PRP include:
- Platelet-derived growth factor (PDGF)
- Transforming growth factor beta (TGF-β)
- Vascular endothelial growth factor (VEGF)
- Insulin-like growth factor (IGF)
These growth factors help regulate:
- Tissue repair signaling
- Cellular communication
- Blood vessel formation
- Inflammatory responses
PRP has been widely used in regenerative medicine and is being studied for its potential role in supporting tissue healing in various organs.
Platelet-Rich Fibrin (PRF)
PRF is another blood-derived regenerative therapy that contains platelets embedded within a fibrin scaffold.
This fibrin network allows growth factors to be released gradually over time, potentially providing sustained biological signaling during tissue repair.
PRF contains:
- Platelets
- Leukocytes (immune cells)
- Cytokines involved in healing
- Growth factors that support tissue repair
Potential biological effects being studied include:
- Sustained release of regenerative signaling molecules
- Support for tissue healing
- Improved cellular communication
- Modulation of inflammatory responses
PRF is increasingly used in regenerative medicine procedures.
Supporting Kidney Health
Managing kidney disease typically involves a combination of medical treatment, lifestyle modifications, and ongoing monitoring.
Important strategies include:
- Managing blood pressure
- Controlling blood sugar levels
- Maintaining healthy hydration
- Reducing sodium intake
- Avoiding nephrotoxic medications when possible
- Maintaining a balanced diet
- Regular medical follow-up and laboratory monitoring
Early detection and management are critical to slowing disease progression.
Frequently Asked Questions
What is the most common cause of kidney disease?
The most common causes are diabetes and high blood pressure, both of which can damage the small blood vessels within the kidneys.
Can kidney disease be reversed?
Some early forms of kidney damage may improve with appropriate treatment and lifestyle changes. However, advanced kidney disease may not be fully reversible.
What is kidney failure?
Kidney failure occurs when the kidneys lose most of their filtering ability. In advanced cases, patients may require dialysis or kidney transplantation.
Are regenerative therapies approved for kidney disease treatment?
Regenerative therapies are an area of active scientific research. Their potential role in supporting kidney repair continues to be studied in clinical trials.
How can kidney disease be detected early?
Routine blood and urine tests can detect early signs of kidney dysfunction, including changes in creatinine levels, glomerular filtration rate (GFR), and urine protein levels.

