Causes, Symptoms, and Emerging Regenerative Treatment Approaches
Understanding Sciatica
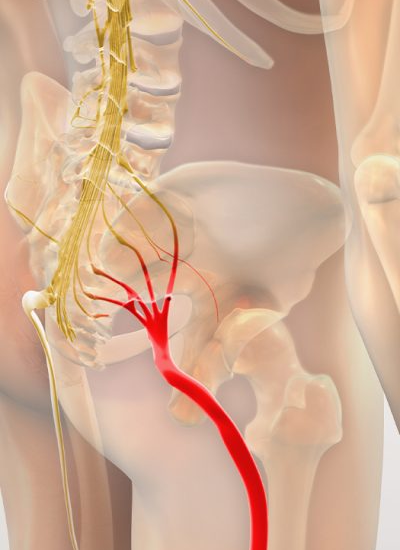
Sciatica is a condition characterized by pain that radiates along the path of the sciatic nerve, which runs from the lower back through the hips and buttocks and down each leg. It occurs when the sciatic nerve becomes compressed, irritated, or inflamed, often due to underlying spinal conditions.
The sciatic nerve is the largest nerve in the human body, formed by nerve roots that exit the lower spine at levels L4, L5, S1, S2, and S3. These nerve roots combine to form a single large nerve that controls sensation and motor function in much of the lower body.
When the nerve becomes irritated or compressed, it can cause symptoms that travel from the lower back into the buttock and down the leg, sometimes reaching the foot or toes.
Sciatica is relatively common and affects millions of individuals worldwide, particularly adults between the ages of 30 and 60. While many cases resolve with conservative treatment, some individuals experience chronic or recurring sciatic nerve pain.
Anatomy of the Sciatic Nerve
The sciatic nerve originates in the lumbar and sacral regions of the spine and passes through several anatomical structures before reaching the legs.
Key anatomical regions include:
- Lumbar spine (lower back)
- Sacral nerve roots
- Piriformis muscle in the buttock
- Posterior thigh
- Branches into the tibial and common peroneal nerves near the knee
Because of its long pathway, compression or irritation can occur at multiple locations along the nerve.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Common Causes of Sciatica
Sciatica is typically caused by an underlying spinal or musculoskeletal condition that places pressure on the sciatic nerve.
Herniated Disc
One of the most common causes of sciatica is a lumbar disc herniation.
Spinal discs act as cushions between vertebrae. Each disc contains a soft inner material (nucleus pulposus) surrounded by a tougher outer layer (annulus fibrosus).
When the outer layer weakens or tears, the inner material can bulge or protrude outward, potentially compressing nearby nerve roots that form the sciatic nerve.
Degenerative Disc Disease
As individuals age, spinal discs gradually lose hydration and elasticity. This process, known as degenerative disc disease, can reduce the space between vertebrae and place pressure on spinal nerves.
Disc degeneration may also contribute to:
- Disc bulging
- Reduced spinal stability
- Nerve irritation
Spinal Stenosis
Spinal stenosis occurs when the spinal canal narrows, placing pressure on nerves within the spine.
This narrowing may result from:
- Age-related degenerative changes
- Bone spurs (osteophytes)
- Thickened ligaments
- Disc degeneration
Lumbar spinal stenosis is a frequent cause of sciatica in older adults.
Piriformis Syndrome
The piriformis muscle, located deep in the buttock, lies close to the sciatic nerve.
If this muscle becomes tight, inflamed, or spasms, it may compress the nerve and cause symptoms similar to sciatica.
Spondylolisthesis
Spondylolisthesis occurs when one vertebra slips forward over the vertebra beneath it. This shift can narrow nerve passageways and compress the sciatic nerve roots.
Trauma or Injury
Falls, sports injuries, or accidents can damage spinal structures and contribute to sciatic nerve compression.
Symptoms of Sciatica
Symptoms may vary depending on the location and severity of nerve compression.
Common symptoms include:
Radiating Leg Pain
Pain often begins in the lower back or buttock and travels down one leg.
The pain may feel:
- Sharp
- Burning
- Electric-like
- Shooting
Numbness and Tingling
Compression of nerve fibers may cause abnormal sensations, including:
- Pins-and-needles
- Numbness
- Reduced sensation in the leg or foot
Muscle Weakness
If motor nerve fibers are affected, individuals may experience:
- Leg weakness
- Difficulty lifting the foot (foot drop)
- Reduced muscle control
Worsening Pain with Movement
Sciatica pain often increases during activities such as:
- Sitting for long periods
- Bending or twisting
- Lifting heavy objects
- Coughing or sneezing
Chronic Sciatica
In some cases, sciatic nerve irritation becomes chronic, lasting for months or years.
Chronic nerve compression may lead to:
- Persistent nerve inflammation
- Reduced nerve conduction
- Muscle weakness
- Limited mobility
- Reduced quality of life
Addressing the underlying cause of nerve compression is often necessary for long-term relief.
Conventional Treatment Options
Many cases of sciatica improve with conservative treatment.
Physical Therapy
Physical therapy programs may include:
- Core strengthening
- Postural correction
- Stretching exercises
- Spinal stabilization techniques
Anti-Inflammatory Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs) may help reduce inflammation and relieve pain.
Corticosteroid Injections
Epidural steroid injections are sometimes used to reduce inflammation around spinal nerves.
While these injections may temporarily relieve symptoms, they do not repair underlying tissue damage.
Surgery
In severe cases involving persistent nerve compression or neurological deficits, surgical procedures may be recommended.
Common procedures include:
- Discectomy (removal of herniated disc material)
- Laminectomy (removal of part of a vertebra to relieve pressure)
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative Medicine and Sciatica
Regenerative medicine focuses on supporting the body’s natural repair processes, particularly in damaged tissues such as spinal discs, ligaments, and nerves.
These therapies aim to improve the biological environment surrounding irritated nerves and injured spinal structures.
Platelet-Rich Plasma (PRP)
PRP is derived from a patient’s own blood and contains concentrated platelets that release growth factors involved in tissue repair.
PRP has been studied in spinal and orthopedic medicine for its potential to:
- Reduce inflammation around compressed nerves
- Support healing of damaged ligaments and soft tissues
- Improve blood supply to injured tissues
- Support disc and connective tissue repair
PRP may be used in targeted injections around affected spinal structures.
Platelet-Rich Fibrin (PRF)
PRF is an advanced platelet therapy that forms a fibrin scaffold capable of slowly releasing growth factors over time.
Potential benefits include:
- Sustained growth factor signaling
- Enhanced tissue repair support
- Improved connective tissue healing
- Reduced local inflammation
PRF may support the healing environment around injured spinal tissues.
Stem Cell Therapy
Stem cells are specialized cells capable of influencing tissue repair through regenerative signaling.
Rather than directly replacing damaged tissues, stem cells primarily act through paracrine signaling, releasing molecules that regulate healing and inflammation.
In spinal conditions, stem cells may support:
- Disc tissue regeneration signaling
- Reduction of inflammatory pathways
- Improved vascular support for damaged tissues
- Nerve repair signaling
Stem cell therapies are being studied for their potential role in degenerative spinal conditions and nerve injuries.
Exosome Therapy
Exosomes are microscopic extracellular vesicles that carry signaling molecules between cells.
They contain:
- Proteins
- Growth factors
- Messenger RNA
- MicroRNA
These molecules help regulate cellular communication during tissue repair.
Potential roles in regenerative medicine include:
- Supporting nerve healing pathways
- Reducing inflammatory signaling
- Enhancing cellular repair mechanisms
- Improving tissue communication during recovery
Exosomes represent an emerging area of regenerative medicine research.
Potential Benefits of Regenerative Therapies
While research is ongoing, regenerative therapies may support:
- Reduced nerve inflammation
- Improved tissue healing
- Enhanced cellular repair signaling
- Support for spinal connective tissue health
- Improved nerve function
These therapies aim to support the biological environment surrounding injured spinal structures and nerves.
Frequently Asked Questions
Does sciatica always require surgery?
Most cases of sciatica improve with conservative treatments such as physical therapy and anti-inflammatory approaches.
How long does sciatica usually last?
Acute sciatica may resolve within several weeks, though chronic cases can last longer if underlying spinal conditions persist.
Can exercise help sciatica?
Appropriate exercises designed to strengthen the core and support spinal alignment may help reduce pressure on the sciatic nerve.
Are regenerative treatments commonly used for sciatica?
Regenerative therapies are being studied in orthopedic and spine medicine for their potential role in tissue repair and inflammation modulation.
Who may be a candidate for regenerative therapies?
Individuals with conditions such as:
- Degenerative disc disease
- Chronic ligament injuries
- Persistent nerve inflammation
may benefit from evaluation by a qualified physician.
Below is a condensed but detailed educational page for Degenerative Disc Disease and Herniated Disc Pain, written in the same structure and tone as the other pages you’ve been creating for your website.

