Causes, Symptoms, and Emerging Regenerative Treatment Approaches
Understanding Osteoarthritis
Osteoarthritis (OA) is the most common form of arthritis, affecting millions of people worldwide. It is a degenerative joint condition that occurs when the protective cartilage that cushions the ends of bones gradually wears down, leading to pain, stiffness, inflammation, and reduced mobility.
Healthy joints contain a smooth layer of cartilage that allows bones to glide over one another with minimal friction. This cartilage also absorbs mechanical stress during movement. In osteoarthritis, this cartilage deteriorates over time, causing the bones within the joint to rub against each other.
The condition most commonly affects weight-bearing joints, particularly:
- Knees
- Hips
- Ankles
However, osteoarthritis may also develop in other joints such as the spine, hands, and shoulders.
Although osteoarthritis is often associated with aging, it can also develop due to injury, repetitive stress, genetics, or biomechanical imbalances. Over time, joint degeneration can significantly impact daily activities, mobility, and overall quality of life.
Joint Anatomy and Cartilage Function
To understand osteoarthritis, it is helpful to understand how healthy joints function.
A normal joint includes several key structures:
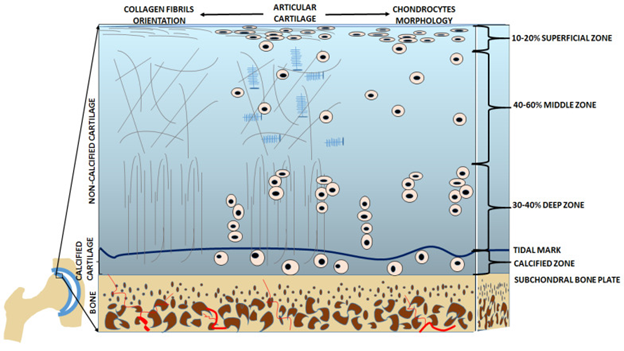
Articular Cartilage
Articular cartilage is a smooth, durable tissue that covers the ends of bones inside joints. It allows bones to move against each other with minimal friction and helps distribute mechanical forces.
Cartilage is composed primarily of:
- Collagen fibers
- Water
- Proteoglycans
- Chondrocytes (cartilage cells)
Because cartilage has very limited blood supply, it has a reduced ability to repair itself after injury or degeneration.
Synovial Fluid
Synovial fluid lubricates joints and provides nutrients to cartilage cells. In osteoarthritis, the composition of synovial fluid may change, contributing to joint inflammation and reduced lubrication.
Subchondral Bone
The bone directly beneath cartilage is known as subchondral bone. As cartilage deteriorates, this bone may become thicker and develop abnormal growths called bone spurs (osteophytes).
How Osteoarthritis Develops
Osteoarthritis develops gradually through a series of biological and structural changes within the joint.
Cartilage Breakdown
The earliest stages of osteoarthritis involve damage to the cartilage matrix. This can occur due to:
- Mechanical stress
- Inflammation
- Age-related degeneration
- Joint injury
Over time, cartilage becomes thinner and loses its smooth surface.
Inflammatory Signaling
Although osteoarthritis is often considered a “wear-and-tear” condition, research shows that inflammatory pathways play a significant role in disease progression.
Inflammatory molecules within the joint can accelerate cartilage breakdown and contribute to pain and swelling.
Bone Changes
As cartilage deteriorates, the body may attempt to stabilize the joint by producing extra bone tissue. This process can lead to the formation of bone spurs, which may further restrict movement and contribute to pain.
Joint Instability
Loss of cartilage and changes in surrounding ligaments and muscles may lead to joint instability and altered movement patterns, further accelerating joint degeneration.
Osteoarthritis of the Knee
The knee is one of the most commonly affected joints because it bears a significant portion of the body’s weight.
Knee osteoarthritis may involve degeneration of cartilage between:
- The femur (thigh bone)
- The tibia (shin bone)
- The patella (kneecap)
Common symptoms include:
- Knee pain during walking or climbing stairs
- Joint stiffness, especially in the morning
- Swelling or inflammation
- Grinding or clicking sensations
- Reduced range of motion
Severe knee osteoarthritis can significantly limit mobility and daily activities.
Osteoarthritis of the Hip
The hip joint is a ball-and-socket joint that supports the upper body during movement. Osteoarthritis of the hip occurs when cartilage between the femoral head and acetabulum gradually deteriorates.
Symptoms may include:
- Deep hip or groin pain
- Pain that radiates into the thigh or buttock
- Stiffness when standing after sitting
- Reduced range of motion
- Difficulty walking or climbing stairs
Hip osteoarthritis may progressively affect balance, posture, and overall mobility.
Osteoarthritis of the Ankle
Although less common than knee or hip osteoarthritis, ankle OA may develop after previous injuries such as fractures or ligament tears.
Symptoms may include:
- Ankle pain during walking
- Joint stiffness
- Swelling
- Reduced stability
- Difficulty with weight-bearing activities
Because the ankle joint experiences high mechanical loads during movement, cartilage damage can significantly impact mobility.
Risk Factors for Osteoarthritis
Several factors increase the risk of developing osteoarthritis.
Aging
Cartilage gradually loses elasticity and resilience over time.
Joint Injury
Previous injuries such as ligament tears or fractures can increase the likelihood of osteoarthritis later in life.
Repetitive Mechanical Stress
Occupations or sports involving repetitive joint loading may contribute to cartilage wear.
Obesity
Excess body weight increases stress on weight-bearing joints, particularly the knees and hips.
Genetics
Some individuals may inherit a predisposition to cartilage degeneration.
Muscle Weakness
Weak muscles surrounding joints can increase joint instability and stress on cartilage.
Conventional Treatment Approaches
Traditional osteoarthritis treatments focus on symptom management and preserving joint function.
Physical Therapy
Exercise programs may strengthen surrounding muscles and improve joint stability.
Anti-Inflammatory Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs) may help reduce pain and inflammation.
Corticosteroid Injections
Steroid injections may temporarily reduce inflammation inside the joint.
Hyaluronic Acid Injections
These injections aim to improve joint lubrication and reduce friction.
Joint Replacement Surgery
In severe cases where cartilage loss is extensive, joint replacement surgery may be recommended.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative Medicine and Joint Health
Regenerative medicine focuses on supporting the body’s natural repair processes, particularly in tissues such as cartilage that have limited regenerative capacity.
These therapies aim to improve the biological environment within the joint and support healing signals.
Platelet-Rich Plasma (PRP)
PRP is produced by concentrating platelets from a patient’s own blood. Platelets release growth factors involved in tissue repair and cellular communication.
PRP may support:
- Reduction of joint inflammation
- Cartilage repair signaling
- Improved joint lubrication
- Enhanced healing of surrounding soft tissues
PRP has been widely studied in orthopedic medicine for osteoarthritis management.
Platelet-Rich Fibrin (PRF)
PRF is an advanced platelet concentrate that forms a fibrin scaffold capable of gradually releasing growth factors over time.
Potential benefits include:
- Sustained growth factor delivery
- Improved tissue repair signaling
- Reduced inflammation
- Support for connective tissue healing
PRF may help support joint tissue repair processes.
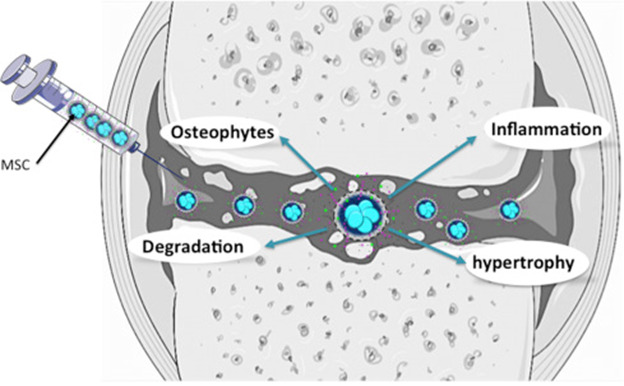
Stem Cell Therapy
Stem cells are specialized cells capable of influencing tissue repair and regeneration.
In orthopedic research, stem cells are being studied for their potential to:
- Support cartilage regeneration signaling
- Modulate inflammation within joints
- Promote tissue repair pathways
- Improve the biological environment for cartilage health
Stem cells primarily work through paracrine signaling, releasing molecules that regulate healing and cellular communication.
Exosome Therapy
Exosomes are microscopic extracellular vesicles released by cells that contain proteins, lipids, and genetic signaling molecules.
They help regulate communication between cells during tissue repair.
Potential roles in joint health include:
- Reducing inflammatory signaling
- Supporting cartilage repair pathways
- Enhancing cellular communication
- Promoting tissue regeneration mechanisms
Exosome therapy is an emerging area of regenerative medicine research.
Potential Benefits of Regenerative Therapies
While research continues to evolve, regenerative therapies may support:
- Reduced joint inflammation
- Improved cartilage repair signaling
- Enhanced healing of surrounding soft tissues
- Improved joint lubrication
- Better joint function and mobility
These therapies aim to optimize the biological environment within degenerating joints.
Frequently Asked Questions
Is osteoarthritis reversible?
Osteoarthritis is generally considered a progressive condition, but treatments may help slow progression and improve joint function.
Can exercise help osteoarthritis?
Yes. Appropriate exercise programs can strengthen muscles around joints and reduce stress on cartilage.
Are regenerative therapies commonly used for osteoarthritis?
PRP and other biologic therapies are increasingly used in orthopedic and sports medicine settings to support joint health.
Can regenerative therapies replace joint replacement surgery?
In some cases they may help manage symptoms and delay surgery, though severe joint damage may still require surgical intervention.
Who may benefit from regenerative treatments?
Individuals experiencing:
- Knee osteoarthritis
- Hip osteoarthritis
- Ankle osteoarthritis
- Chronic joint inflammation
may benefit from evaluation by a qualified physician.

