Understanding Cardiovascular Disease
Cardiovascular disease (CVD) refers to a group of conditions that affect the heart and blood vessels. It is the leading cause of death worldwide and includes a range of disorders involving impaired blood flow, structural heart abnormalities, and damage to the vascular system.
The cardiovascular system is responsible for delivering oxygen, nutrients, hormones, and immune cells throughout the body. When the heart or blood vessels become damaged or diseased, circulation can be compromised, potentially leading to serious complications such as heart attacks, stroke, heart failure, and peripheral vascular disease.
Cardiovascular disease often develops gradually over many years and is frequently associated with chronic inflammation, oxidative stress, metabolic dysfunction, and vascular damage.
In addition to conventional treatments such as medications, lifestyle modification, and surgical interventions, regenerative medicine therapies including stem cells, exosomes, platelet-rich plasma (PRP), and platelet-rich fibrin (PRF) are being studied for their potential role in supporting cardiovascular repair and vascular regeneration.
Types of Cardiovascular Disease
Cardiovascular disease includes several related conditions affecting the heart and vascular system.
Coronary Artery Disease
Coronary artery disease occurs when the arteries that supply blood to the heart become narrowed or blocked due to atherosclerosis, a buildup of plaque composed of cholesterol, inflammatory cells, and fatty deposits.
This reduced blood flow can lead to:
- Chest pain (angina)
- Shortness of breath
- Heart attack (myocardial infarction)
Contact Us
Heart Failure
Heart failure occurs when the heart is unable to pump blood effectively to meet the body’s needs.
This may develop due to:
• Previous heart attacks
• Long-standing high blood pressure
• Cardiomyopathy
• Valve disorders
Symptoms may include fatigue, fluid retention, swelling in the legs, and difficulty breathing.
Cardiomyopathy
Cardiomyopathy refers to diseases of the heart muscle itself, which may cause the heart to become enlarged, thickened, or weakened.
Common types include:
• Dilated cardiomyopathy
• Hypertrophic cardiomyopathy
• Restrictive cardiomyopathy
These conditions can interfere with the heart’s ability to pump blood effectively.
Peripheral Artery Disease
Peripheral artery disease (PAD) occurs when arteries supplying the limbs become narrowed, reducing blood flow to the legs and feet.
Symptoms may include:
• Leg pain while walking
• Numbness or weakness in the limbs
• Slow wound healing
• Cold extremities
Stroke and Cerebrovascular Disease
When blood flow to the brain becomes interrupted, brain tissue can be damaged due to lack of oxygen. This may occur due to a blood clot or a ruptured blood vessel.
Stroke is a major complication associated with cardiovascular disease.
Causes and Risk Factors
Cardiovascular disease is influenced by a combination of genetic, metabolic, and lifestyle factors.
Common risk factors include:
• High blood pressure
• High cholesterol
• Diabetes
• Smoking
• Obesity
• Sedentary lifestyle
• Chronic inflammation
• Poor diet
• Chronic stress
• Family history of heart disease
Many of these factors contribute to vascular inflammation and plaque formation, which gradually damages arteries and restricts blood flow.
The Role of Inflammation and Vascular Damage
A growing body of research suggests that chronic inflammation plays a central role in cardiovascular disease.
Inflammation within the arterial walls can:
• Damage endothelial cells (the cells lining blood vessels)
• Promote plaque formation
• Trigger blood clot formation
• Reduce nitric oxide production, impairing blood vessel relaxation
Over time, these processes contribute to atherosclerosis, the primary underlying cause of many cardiovascular conditions.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative Medicine and Cardiovascular Health
Regenerative medicine focuses on supporting the body’s natural repair mechanisms through the use of biological therapies that may promote tissue regeneration, cellular signaling, and vascular repair.
While research is ongoing, therapies such as stem cells, exosomes, PRP, and PRF are being investigated for their potential ability to support cardiovascular function and tissue repair.
These therapies aim to improve cellular communication, reduce inflammation, and promote regeneration of damaged tissues.
Stem Cell Therapy for Cardiovascular Conditions
Stem cells are undifferentiated cells capable of developing into specialized tissue cells.
In cardiovascular medicine, mesenchymal stem cells (MSCs) and other progenitor cells are being studied for their potential ability to support heart tissue repair and vascular regeneration.
Potential mechanisms being investigated include:
• Supporting the formation of new blood vessels (angiogenesis)
• Releasing growth factors that stimulate tissue repair
• Reducing inflammatory signaling
• Improving blood vessel function
• Supporting cardiac muscle cell survival
Researchers are particularly interested in stem cells for conditions such as heart failure, ischemic heart disease, and cardiomyopathy.
Exosome Therapy
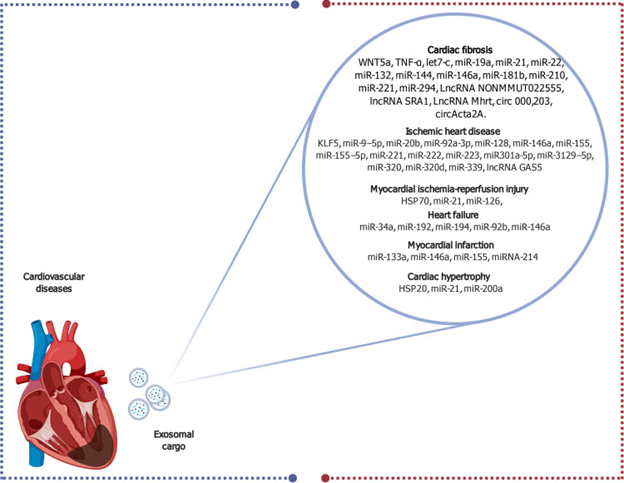
Exosomes are tiny extracellular vesicles released by cells that contain proteins, lipids, RNA molecules, and signaling factors.
They play an important role in cell-to-cell communication, allowing cells to send signals that influence healing and regeneration.
In cardiovascular research, exosomes are being studied for their potential to:
• Support vascular repair
• Improve endothelial cell function
• Promote angiogenesis
• Reduce inflammation in blood vessels
• Improve mitochondrial function in heart cells
Because exosomes contain signaling molecules rather than whole cells, they are being explored as a potential way to deliver regenerative signals to damaged tissues.
Platelet-Rich Plasma (PRP)
PRP is a concentration of platelets derived from the patient’s own blood.
Platelets contain numerous growth factors that play a role in tissue repair and vascular health, including:
• Platelet-derived growth factor (PDGF)
• Vascular endothelial growth factor (VEGF)
• Transforming growth factor beta (TGF-β)
• Insulin-like growth factor (IGF)
These growth factors help regulate processes such as:
• Tissue repair
• Blood vessel formation
• Cellular signaling
• Inflammatory modulation
PRP is widely used in regenerative medicine and is being studied for its role in supporting tissue healing in a variety of medical fields.
Platelet-Rich Fibrin (PRF)
PRF is a blood-derived regenerative therapy that contains platelets embedded in a fibrin matrix, which acts as a natural scaffold.
This fibrin network allows for the slow release of growth factors over time, potentially supporting sustained tissue repair signaling.
PRF contains:
• Platelets
• Leukocytes (immune cells)
• Cytokines and growth factors
Potential biological effects being studied include:
• Improved tissue regeneration signaling
• Enhanced vascular repair
• Support for extracellular matrix formation
• Reduced inflammatory signaling
PRF has been widely used in regenerative procedures and is being investigated in various fields of medicine.
Supporting Cardiovascular Health
In addition to medical treatment, several lifestyle factors play a critical role in cardiovascular health.
Important strategies include:
• Maintaining a heart-healthy diet
• Regular physical activity
• Controlling blood pressure and cholesterol
• Managing blood sugar levels
• Reducing chronic stress
• Avoiding smoking
Addressing these factors can significantly reduce the risk of cardiovascular complications.
Frequently Asked Questions
What is the most common cause of cardiovascular disease?
The most common cause is atherosclerosis, a condition in which plaque builds up inside the arteries, restricting blood flow.
Can cardiovascular disease be reversed?
While advanced disease may not always be completely reversible, lifestyle changes and appropriate medical care can significantly slow disease progression and improve heart health.
What role does inflammation play in heart disease?
Chronic inflammation contributes to damage within blood vessels, promoting plaque buildup and increasing the risk of heart attack and stroke.
Are regenerative therapies approved for cardiovascular disease?
Regenerative therapies are an area of active scientific research. Their potential role in cardiovascular care continues to be studied in clinical trials.
Can regenerative medicine replace traditional heart treatments?
No. Standard treatments such as medications, lifestyle modification, and surgical procedures remain essential components of cardiovascular care.
Are There FDA-Approved Treatments Using Stem Cells for CVD?
There are currently no FDA-approved stem cell therapies for cardiovascular disease (CVD). However, some investigational therapies have received the FDA’s Breakthrough Therapy designation, which allows for an expedited development and review process during research. This designation does not indicate that a therapy has been approved.
What’s Most Dangerous About CVD?
At its core, cardiovascular disease can affect blood flow throughout the body. Blood carries oxygen, nutrients, and waste products, so reduced or blocked circulation may lead to damage to tissues or organs. Individuals who have concerns or possible symptoms related to cardiovascular health are generally encouraged to seek evaluation from qualified healthcare professionals.
How Promising Does PRP and PRF Look for CVD?
Both platelet-rich plasma (PRP) and platelet-rich fibrin (PRF) are being explored in research settings. In laboratory studies, PRP and PRF have demonstrated the presence of growth factors that may support natural healing processes. Their potential role in cardiovascular conditions remains investigational, and further research is needed to better understand safety and effectiveness.
Could Experimental Therapies Become Cardiovascular Disease Prevention?
It is possible that ongoing research into experimental therapies may contribute to future approaches to cardiovascular disease prevention. At present, most studies focus on understanding disease progression and exploring ways to slow or manage it. Whether any investigational therapy could play a role in prevention will depend on future research findings and regulatory evaluation.
How Can People Access Investigative Therapies?
The only way to access most investigative therapies is to join a clinical trial. The options to receive stem cells for cardiovascular disease in Long Island are mostly available at the research hospitals in the city. People should be aware that trials require control groups, so even if they are accepted into a trial, there’s no guarantee they’ll receive the experimental treatment.