Immune Dysregulation, Loss of Self-Tolerance, Multisystem Inflammation, and Regenerative Therapeutic Science
Overview
Systemic Lupus Erythematosus (SLE) is a chronic, relapsing–remitting autoimmune disease characterized by loss of immune tolerance, production of pathogenic autoantibodies, immune complex deposition, and widespread inflammatory tissue injury. SLE affects multiple organ systems simultaneously, including the skin, joints, kidneys, cardiovascular system, nervous system, and hematologic compartments.
Rather than a single disease, SLE is increasingly understood as a heterogeneous immune dysregulation syndrome, with variable genetic susceptibility, immune phenotypes, and end-organ manifestations.
Core Pathophysiology
1. Loss of Immune Tolerance & Autoantibody Production
At the center of SLE is a failure of immune self-recognition:
- Defective central and peripheral tolerance
- Impaired regulatory T-cell (Treg) function
- Hyperactive B-cell differentiation and survival
- Production of pathogenic autoantibodies (ANA, anti-dsDNA, anti-Smith, antiphospholipid antibodies)
These autoantibodies form immune complexes that circulate and deposit in tissues.
2. Immune Complex Deposition & Complement Activation
Immune complexes trigger:
- Complement activation (C3, C4 consumption)
- Recruitment of neutrophils and macrophages
- Release of proteolytic enzymes and reactive oxygen species
This process drives direct tissue injury, particularly in:
- Kidneys (lupus nephritis)
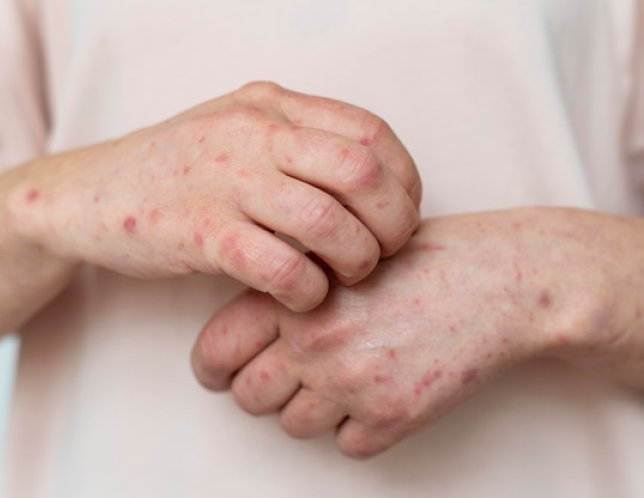
- Skin (cutaneous lupus)
- Joints
- Blood vessels
3. Type I Interferon Pathway Dysregulation
SLE is strongly associated with chronic activation of the Type I interferon (IFN-α) pathway.
Key effects:
- Amplification of B-cell autoantibody production
- Enhanced antigen presentation
- Sustained immune activation
- Suppression of immune resolution mechanisms
The “interferon signature” is now considered a core disease driver, not a secondary phenomenon.
4. Innate Immune Activation & NETosis
Neutrophils in SLE demonstrate increased NETosis (release of neutrophil extracellular traps):
- Exposes nuclear antigens
- Further stimulates autoantibody production
- Promotes endothelial injury and thrombosis
- Perpetuates inflammation
This links autoimmunity, vascular injury, and thrombosis.
5. Endothelial Dysfunction & Vascular Inflammation
SLE is associated with accelerated vascular aging:
- Endothelial nitric oxide dysfunction
- Immune-mediated vasculitis
- Increased arterial stiffness
- Microvascular inflammation
This contributes to:
- Premature atherosclerosis
- Increased cardiovascular morbidity
- End-organ ischemia
Cardiovascular disease is a leading cause of mortality in SLE.
6. Neuroimmune & Central Nervous System Involvement
Neuropsychiatric lupus reflects immune-mediated nervous system injury:
- Blood–brain barrier disruption
- Autoantibody penetration into CNS
- Microglial activation
- Cytokine-mediated neuronal dysfunction
Manifestations include:
- Cognitive dysfunction
- Headache
- Mood disorders
- Seizures
- Autonomic dysregulation
7. Mitochondrial Dysfunction & Energetic Failure
Chronic immune activation in SLE is associated with:
- Increased oxidative stress
- Impaired mitochondrial respiration
- Reduced ATP production
This contributes to:
- Profound fatigue
- Exercise intolerance
- Poor tissue recovery
- Heightened inflammatory sensitivity
Clinical Manifestations
SLE presents with variable combinations of:
- Fatigue and malaise
- Inflammatory arthritis
- Photosensitive rashes
- Oral ulcers
- Serositis
- Cytopenias
- Renal involvement
- Neurologic and psychiatric symptoms
- Thrombotic complications
Disease course is typically relapsing and unpredictable, with periods of remission and flare.
Limitations of Conventional Management
Standard therapies include:
- Corticosteroids
- Antimalarials (hydroxychloroquine)
- Immunosuppressive agents
- Biologic immune modulators
While these therapies:
- Reduce disease activity
- Prevent acute organ damage
They do not:
- Restore immune tolerance
- Reverse accumulated tissue injury
- Fully address chronic inflammation
- Correct mitochondrial or vascular dysfunction
Long-term treatment is often limited by toxicity and cumulative side effects.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative & Biologic Therapeutic Concepts
(Investigational / Adjunctive – Not FDA-approved for SLE)
Immune Rebalancing & Resolution Signaling (Research-Based)
Emerging research focuses on:
- Enhancing regulatory immune pathways
- Shifting macrophage phenotypes toward resolution
- Modulating interferon signaling without global immunosuppression
The goal is immune recalibration, not immune suppression.
Platelet-Derived Biologics (PRP / PRF – Investigational)
Autologous platelet concentrates contain growth factors and cytokine modulators that may:
- Support tissue repair in chronically inflamed environments
- Improve microvascular signaling
- Modulate local inflammatory responses
- Enhance connective tissue resilience
Their relevance in SLE is theoretical and adjunctive, not disease-modifying.
Mesenchymal Stromal Cell & Exosome Research
Current research explores:
- MSC-mediated immune modulation
- Reduction of autoantibody-driven inflammation
- Exosome-based delivery of regulatory microRNAs
- Endothelial and mitochondrial support
Observed effects in preclinical and early clinical studies include:
- Reduced inflammatory cytokines
- Improved vascular function
- Attenuation of immune-mediated tissue injury
Supportive Adjunctive Modalities
Often explored alongside medical therapy:
- Photobiomodulation (mitochondrial support)
- Hyperbaric oxygen therapy (microvascular optimization)
- Autonomic nervous system regulation
- Metabolic and micronutrient optimization
These approaches aim to reduce systemic inflammatory burden, not replace immunologic treatment.
Clinical Perspective
SLE is best understood as:
- A systemic immune tolerance disorder
- With chronic inflammatory, vascular, and neurologic consequences
- Requiring long-term, individualized management
Future strategies emphasize:
- Immune tolerance restoration
- Inflammation resolution
- Vascular protection
- Organ-specific preservation
- Biologic repair signaling
Summary
- SLE is driven by loss of immune tolerance and autoantibody formation
- Type I interferon signaling is a central disease mechanism
- Immune complex deposition causes multisystem injury
- Vascular and mitochondrial dysfunction contribute to morbidity
- Conventional therapies control flares but are not curative
Regenerative and immune-modulating strategies remain investigational but conceptually promising

