Persistent Immune Activation, Neuroinflammation, Immune Evasion, and Regenerative Therapeutic Science
Overview
Lyme disease is a multisystem, tick-borne infectious disease caused primarily by Borrelia burgdorferi, a highly immune-evasive spirochete. While early infection may respond to antibiotic therapy, a subset of patients develop persistent symptoms despite appropriate treatment, commonly referred to as Post-Treatment Lyme Disease Syndrome (PTLDS).
Lyme disease is increasingly recognized not only as an infection, but as a condition capable of triggering chronic immune dysregulation, neuroinflammation, autonomic dysfunction, and multisystem inflammatory injury, even after microbial burden is reduced.
Core Pathophysiology
1. Immune Evasion & Persistent Antigenic Stimulation
Borrelia burgdorferi possesses unique survival mechanisms:
- Ability to alter surface antigens (antigenic variation)
- Formation of biofilm-like aggregates
- Intracellular and immune-privileged tissue localization
- Downregulation of host immune clearance pathways
These mechanisms may result in persistent antigen exposure, even in the absence of active infection, driving ongoing immune activation.
2. Innate & Adaptive Immune Dysregulation
Lyme disease activates both innate and adaptive immune pathways:
- Toll-like receptor (TLR) activation
- Macrophage and dendritic cell stimulation
- Th1 and Th17 skewed immune responses
- Impaired regulatory T-cell (Treg) balance
This immune imbalance can persist beyond acute infection, leading to chronic inflammatory signaling rather than immune resolution.

3. Cytokine-Driven Inflammation
Patients with persistent symptoms often demonstrate elevations in:
- IL-6
- IL-8
- TNF-α
- IFN-γ
These cytokines contribute to:
- Fatigue and sickness behavior
- Central and peripheral pain sensitization
- Cognitive dysfunction (“brain fog”)
- Impaired mitochondrial energy production
The result is a systemic inflammatory state, not limited to a single organ.
4. Neuroinflammation & Nervous System Involvement
Lyme disease commonly affects the nervous system:
- Peripheral neuropathy
- Cranial neuropathies
- Radiculopathy
- Cognitive and mood disturbances
- Autonomic dysfunction (POTS-like features)
Mechanisms include:
- Blood–brain barrier disruption
- Microglial activation
- Immune-mediated neural injury
- Neurotoxic inflammatory metabolites
This supports the concept of Lyme disease as a neuroimmune disorder, not simply an infectious one.
5. Mitochondrial Dysfunction & Energetic Failure
Chronic inflammation and immune activation impair cellular energy systems:
- Reduced mitochondrial oxidative phosphorylation
- Increased reactive oxygen species
- Impaired ATP production
This contributes to:
- Severe fatigue
- Exercise intolerance
- Post-exertional symptom exacerbation
- Cognitive slowing
These features overlap with other post-inflammatory syndromes.
6. Autoimmune-Like Sequelae
In some patients, Lyme disease appears to trigger immune cross-reactivity:
- Molecular mimicry between bacterial antigens and host tissues
- Autoantibody formation
- Persistent immune activation without detectable infection
This may explain long-term musculoskeletal pain, neurologic symptoms, and inflammatory arthritis in certain individuals.
Clinical Manifestations
Lyme disease presents across a spectrum:
Early Disease
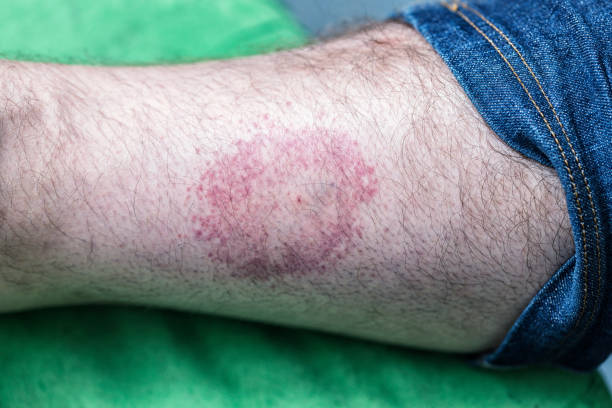
- Erythema migrans rash
- Flu-like symptoms
- Arthralgia
- Headache and neck stiffness
Disseminated / Persistent Symptoms
- Chronic fatigue
- Neuropathic pain
- Cognitive dysfunction
- Autonomic instability
- Migratory joint pain
- Mood and sleep disturbances
Symptoms often fluctuate and may involve multiple organ systems simultaneously.
Limitations of Conventional Management
Standard treatment focuses on:
- Antibiotic therapy for acute infection
- Symptom management
However, in PTLDS:
- Antibiotics may not address immune dysregulation
- Persistent inflammation may continue despite microbial clearance
- Neuroimmune and autonomic dysfunction remain untreated
This has led to increasing interest in immune-modulating and regenerative approaches.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative & Biologic Therapeutic Concepts
(Investigational / Adjunctive – Not FDA-approved for Lyme Disease)
Immune Modulation & Inflammation Control (Research-Based)
Emerging approaches aim to:
- Shift immune signaling from pro-inflammatory to regulatory
- Reduce chronic cytokine activation
- Support immune resolution rather than suppression
These strategies focus on immune balance, not antimicrobial action.
Platelet-Derived Biologics (PRP / PRF – Investigational)
PRP and PRF contain growth factors and cytokine modulators that may:
- Support tissue repair in inflamed environments
- Modulate inflammatory signaling
- Improve microvascular perfusion
- Support nerve and connective tissue resilience
Their role in Lyme-related inflammation is theoretical and investigational, not curative.
Exosome & Extracellular Vesicle Research
Exosomes are being studied for their ability to:
- Deliver anti-inflammatory microRNAs
- Modulate macrophage phenotype
- Support neural and mitochondrial recovery
- Improve endothelial and microvascular function
Preclinical data suggests relevance in post-inflammatory and neuroimmune conditions.
Supportive & Adjunctive Modalities
Often explored in integrative care models:
- Photobiomodulation (mitochondrial and neural support)
- Hyperbaric oxygen therapy (tissue oxygenation and microvascular support)
- Autonomic nervous system regulation
- Nutritional and metabolic optimization
These approaches aim to reduce systemic inflammatory burden, not replace standard medical care.
Clinical Perspective
Lyme disease—particularly persistent or post-treatment syndromes—is increasingly understood as:
- A chronic immune-mediated inflammatory condition
- With neurologic, autonomic, and mitochondrial involvement
- That may persist independently of active infection
Future care models emphasize:
- Immune recalibration
- Neuroinflammation reduction
- Tissue and mitochondrial support
- System-level recovery, rather than pathogen eradication alone
Summary
- Lyme disease can initiate long-lasting immune dysregulation
- Persistent symptoms may reflect inflammation, not active infection
- Neuroimmune and mitochondrial dysfunction are central mechanisms
- Conventional therapies may not address post-infectious biology
Regenerative and biologic approaches remain investigational but conceptually promising