Causes, Symptoms, and Emerging Regenerative Treatment Approaches
Understanding Osteoporosis
Osteoporosis is a progressive skeletal disease characterized by reduced bone density, deterioration of bone microarchitecture, and increased risk of fractures. The condition develops when the balance between bone formation and bone resorption becomes disrupted, leading to fragile bones that break more easily.
Bone is a living, dynamic tissue that constantly undergoes remodeling. Specialized cells called osteoblasts build new bone, while osteoclasts break down old bone. In healthy individuals, these processes remain balanced. In osteoporosis, however, bone resorption begins to exceed bone formation.
Over time, this imbalance leads to thinning of bone tissue and weakening of bone structure, making bones more susceptible to fractures, particularly in the:
- Spine (vertebrae)
- Hip
- Wrist
- Pelvis
Osteoporosis is often referred to as a “silent disease” because bone loss occurs gradually and may not cause symptoms until a fracture occurs.
Globally, osteoporosis affects hundreds of millions of people, with women over the age of 50 at particularly high risk due to hormonal changes associated with menopause.
Bone Biology and the Development of Osteoporosis
Understanding how osteoporosis develops requires an appreciation of bone remodeling and cellular signaling pathways.
Bone Remodeling
Bone remodeling is a continuous process involving:
- Osteoblasts: cells responsible for bone formation
- Osteoclasts: cells responsible for bone breakdown
- Osteocytes: mature bone cells that regulate mineral balance and structural integrity
During youth and early adulthood, bone formation generally exceeds bone breakdown, allowing individuals to build peak bone mass.
After approximately age 30–35, bone resorption gradually begins to outpace bone formation, resulting in age-related bone loss.
Hormonal Regulation
Hormones play a critical role in maintaining bone health.
Estrogen, in particular, helps regulate osteoclast activity. When estrogen levels decline during menopause, osteoclast activity increases, accelerating bone breakdown.
Other hormones involved in bone metabolism include:
- Parathyroid hormone (PTH)
- Vitamin D
- Calcitonin
- Growth hormone
- Testosterone
Disruptions in these hormonal systems can significantly affect bone density.
Bone Microarchitecture
Healthy bone contains a network of interconnected structures known as trabecular bone, which helps distribute mechanical forces.
In osteoporosis:
- Trabeculae become thinner
- Structural connections weaken
- Bone becomes more porous
This structural deterioration significantly increases fracture risk.
Types of Osteoporosis
Primary Osteoporosis
Primary osteoporosis develops naturally with aging and hormonal changes.
It includes:
Postmenopausal Osteoporosis
- Caused by decreased estrogen levels
- More common in women
- Accelerated bone loss occurs during the first 5–10 years after menopause
Age-Related (Senile) Osteoporosis
- Occurs in both men and women
- Associated with reduced osteoblast activity and decreased calcium absorption
Secondary Osteoporosis
Secondary osteoporosis occurs as a result of underlying medical conditions or medications.
Common causes include:
- Long-term corticosteroid use
- Thyroid disorders
- Kidney disease
- Rheumatoid arthritis
- Chronic inflammatory diseases
- Malabsorption disorders
- Certain cancer treatments
Symptoms and Complications
Osteoporosis often develops without noticeable symptoms until a fracture occurs.
Common complications include:
Fragility Fractures
These fractures occur from minor trauma that would not normally break healthy bone.
Common fracture sites include:
- Hip fractures
- Vertebral compression fractures
- Wrist fractures
Vertebral Compression Fractures
When vertebrae collapse due to weakened bone, patients may experience:
- Sudden back pain
- Loss of height
- Forward spinal curvature (kyphosis)
- Reduced mobility
Multiple compression fractures can significantly impact quality of life and physical function.
Reduced Mobility and Independence
Severe fractures can lead to:
- Chronic pain
- Reduced physical activity
- Increased fall risk
- Loss of independence in older adults
Hip fractures in particular are associated with increased mortality and long-term disability.
Risk Factors for Osteoporosis
Several factors increase the likelihood of developing osteoporosis.
Age
Bone density naturally decreases with age.
Hormonal Changes
Postmenopausal women are at significantly higher risk due to decreased estrogen levels.
Genetics
Family history plays an important role in determining bone density and fracture risk.
Nutritional Deficiencies
Low intake of calcium, vitamin D, and protein may contribute to bone loss.
Sedentary Lifestyle
Weight-bearing exercise helps maintain bone density.
Lack of physical activity can accelerate bone weakening.
Medical Conditions
Certain conditions can affect bone metabolism, including:
- Diabetes
- Thyroid disorders
- Gastrointestinal diseases
- Chronic kidney disease
Medications
Long-term use of medications such as corticosteroids may significantly reduce bone density.
Conventional Treatment Approaches
Conventional osteoporosis treatment focuses on slowing bone loss and reducing fracture risk.
Calcium and Vitamin D
Adequate calcium and vitamin D intake supports bone mineralization and overall skeletal health.
Medications
Several medications are used to reduce bone loss or stimulate bone formation.
These may include:
- Bisphosphonates
- Selective estrogen receptor modulators
- Hormone replacement therapy
- Parathyroid hormone analogs
While these medications can improve bone density, they may also carry potential side effects and may not fully restore healthy bone architecture.
Lifestyle Interventions
Lifestyle changes often recommended include:
- Weight-bearing exercise
- Strength training
- Fall prevention strategies
- Smoking cessation
- Limiting excessive alcohol consumption
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative Medicine and Bone Health
Regenerative medicine focuses on supporting the body’s natural repair mechanisms and may offer promising approaches for improving bone healing and skeletal tissue health.
These therapies are being studied for their potential roles in bone regeneration, fracture healing, and cellular signaling.
Platelet-Rich Plasma (PRP)
PRP is created by concentrating platelets from a patient’s own blood. Platelets release growth factors that influence tissue repair and cellular regeneration.
In bone-related conditions, PRP may support:
- Osteoblast activity (bone-forming cells)
- Bone matrix production
- Local blood vessel formation
- Improved fracture healing
- Reduced inflammation around injured bone tissue
PRP has been used in orthopedic and dental procedures to help support bone healing.
Platelet-Rich Fibrin (PRF)
PRF is an advanced form of platelet therapy that creates a fibrin matrix capable of slowly releasing growth factors over time.
This sustained delivery may support:
- Bone regeneration signaling
- Collagen matrix formation
- Angiogenesis (formation of new blood vessels)
- Improved tissue integration during healing
PRF is commonly used in oral surgery, orthopedics, and regenerative procedures involving bone tissue.
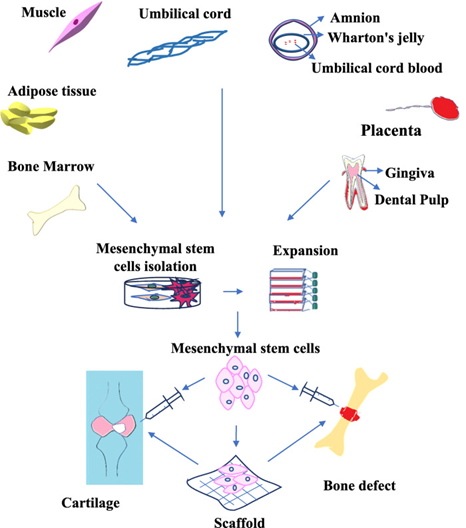
Stem Cell Therapy
Stem cells possess the ability to differentiate into multiple cell types and release bioactive signaling molecules that influence tissue repair.
In bone health, stem cells may support:
- Differentiation into osteoblast-like cells
- Bone matrix regeneration
- Modulation of inflammatory signaling
- Improved vascular supply to healing bone tissue
Stem cell–based therapies are actively being studied for bone regeneration and fracture repair, particularly in cases of delayed healing.
Exosome Therapy
Exosomes are small extracellular vesicles released by cells that contain proteins, lipids, and genetic signaling molecules.
They play an important role in cell-to-cell communication during tissue repair.
Potential roles in bone health include:
- Supporting osteoblast differentiation
- Enhancing cellular signaling involved in bone remodeling
- Reducing inflammatory pathways
- Promoting angiogenesis and tissue repair
Exosomes are an emerging area of regenerative medicine research.
Potential Benefits of Regenerative Therapies
While research continues to evolve, regenerative approaches may support:
- Improved bone healing
- Enhanced fracture recovery
- Increased cellular signaling for bone repair
- Reduced inflammation in injured bone tissue
- Improved vascular support for bone regeneration
These therapies aim to support the biological processes involved in bone maintenance and repair.
Frequently Asked Questions
Can osteoporosis be reversed?
Osteoporosis cannot always be fully reversed, but treatments may help slow bone loss and improve bone density.
How is osteoporosis diagnosed?
Diagnosis is typically made using a bone mineral density test, commonly performed using a DEXA scan.
Who should be screened for osteoporosis?
Screening is generally recommended for:
- Women over age 65
- Postmenopausal women with risk factors
- Men over age 70
- Individuals with a history of fractures
Are regenerative therapies widely used for osteoporosis?
Regenerative therapies are being studied for their potential role in bone healing and skeletal regeneration, but research is ongoing.
Can regenerative treatments replace traditional osteoporosis medications?
These therapies may be used as part of a broader treatment strategy depending on a patient’s medical condition and physician guidance.
Below is a condensed but detailed educational page for Sciatica, written in the same structure and tone as the other pages you’ve been building for your website.

