Understanding Bone Fractures
A bone fracture occurs when a bone breaks or cracks due to trauma, overuse, or underlying bone weakness. Fractures can result from falls, sports injuries, car accidents, repetitive stress, or conditions that weaken bone such as osteoporosis.
Bones are living tissues that constantly remodel themselves through the activity of specialized cells. When a fracture occurs, the body initiates a complex and highly coordinated healing process designed to restore the bone’s structural strength and function. While many fractures heal naturally with proper immobilization, some fractures heal slowly or incompletely, particularly in older individuals or those with underlying health conditions.
Regenerative medicine therapies including stem cells, exosomes, platelet-rich plasma (PRP), and platelet-rich fibrin (PRF) are increasingly being studied for their ability to support the biological processes involved in bone healing.
Types of Bone Fractures
Fractures vary widely depending on the type of injury and the force applied to the bone.
Common fracture types include
Closed fractures – The bone breaks but does not penetrate the skin.
Open (compound) fractures – The bone breaks through the skin and carries a higher risk of infection.
Stress fractures – Small cracks that develop over time from repetitive stress or overuse.
Comminuted fractures – The bone shatters into multiple fragments.
Certain fractures may also be classified as non-union fractures, meaning the bone fails to heal properly after several months.
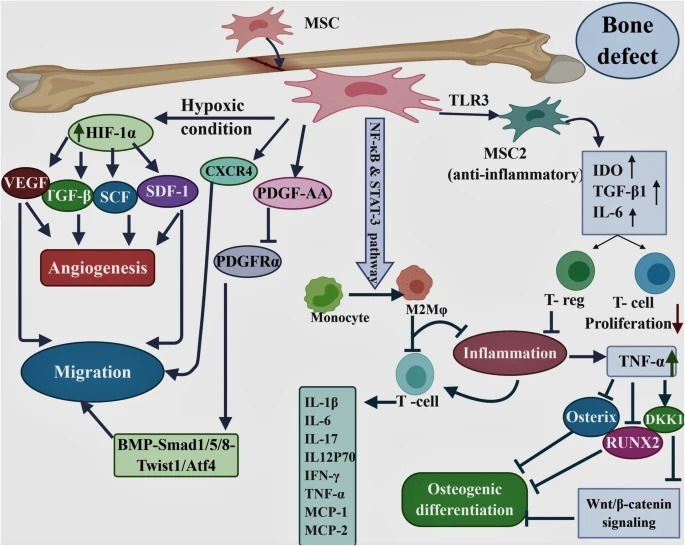
The Biology of Bone Healing
Bone healing occurs in several distinct stages that involve inflammation, tissue regeneration, and structural remodeling.
1. Inflammatory Phase
Immediately after a fracture occurs, blood vessels within the bone rupture, forming a clot known as a fracture hematoma. This clot contains inflammatory cells and growth factors that initiate the healing process.
Immune cells release signaling molecules that attract stem cells and bone-forming cells to the injury site.
2. Soft Callus Formation
Within the first few weeks, specialized cells called chondrocytes and fibroblasts begin forming a soft cartilage-like structure known as a callus around the fracture site.
This callus stabilizes the bone fragments and acts as a scaffold for new bone formation.
3. Hard Callus Formation
Osteoblasts begin depositing new bone tissue, gradually replacing the soft callus with mineralized bone. This stage typically occurs over several weeks to months.
4. Bone Remodeling
Over time, the body reshapes the newly formed bone to restore the bone’s original structure and strength. Osteoclasts remove excess bone while osteoblasts refine the structure.
This remodeling process can continue for months to years.
Factors That Can Delay Bone Healing
Certain conditions can interfere with the normal healing process.
These include:
• Poor blood supply
• Smoking
• Diabetes
• Advanced age
• Nutritional deficiencies
• Severe trauma
• Infection
• Osteoporosis
• Chronic inflammation
Delayed healing can lead to non-union or delayed-union fractures, which may require additional medical intervention.
Individuals seeking further information may contact us to discuss whether a consultation with a physician would be appropriate
Contact Us
Regenerative Medicine and Bone Healing
Regenerative medicine therapies are being studied for their ability to enhance the natural biological processes involved in tissue repair. These therapies aim to support the body’s ability to regenerate bone and surrounding tissues by providing growth factors, signaling molecules, and cellular support.
While research is ongoing, these treatments are being explored as potential adjunctive therapies for certain orthopedic conditions.
Stem Cell Therapy for Bone Repair
Stem cells are undifferentiated cells capable of developing into specialized cell types involved in tissue repair.
In orthopedic medicine, mesenchymal stem cells (MSCs) are of particular interest because they have the potential to develop into bone-forming cells known as osteoblasts.
Stem cells may support bone healing through several mechanisms:
• Differentiating into bone-forming cells
• Releasing growth factors that stimulate bone regeneration
• Reducing inflammation at the injury site
• Supporting blood vessel formation (angiogenesis)
• Enhancing communication between repair cells
Research is ongoing to better understand how stem cell therapies may support fracture healing, particularly in cases of delayed healing or non-union fractures.
Exosome Therapy
Exosomes are microscopic vesicles released by cells that function as cell-to-cell communication signals. They carry proteins, growth factors, and regulatory molecules that influence tissue repair processes.
In bone healing, exosomes are being studied for their ability to:
• Support osteoblast activity
• Regulate inflammation at the injury site
• Enhance cellular communication during repair
• Promote vascular regeneration
• Support tissue remodeling
Because exosomes contain signaling molecules rather than living cells, they are being investigated as a potential method of delivering regenerative signals without introducing new cells.
Platelet-Rich Plasma (PRP)
PRP is created from a patient’s own blood through a process that concentrates platelets and the growth factors they contain.
Platelets release biologically active molecules that play a role in tissue repair and regeneration.
PRP contains important growth factors such as:
• Platelet-derived growth factor (PDGF)
• Transforming growth factor beta (TGF-β)
• Vascular endothelial growth factor (VEGF)
• Insulin-like growth factor (IGF)
These growth factors may support bone healing by:
• Stimulating cell recruitment to the injury site
• Supporting collagen and extracellular matrix formation
• Promoting blood vessel growth
• Enhancing early stages of tissue repair
PRP is commonly studied in orthopedic medicine for soft tissue injuries and bone healing support.
Platelet-Rich Fibrin (PRF)
PRF is another blood-derived regenerative therapy that contains platelets embedded within a fibrin matrix. Unlike PRP, PRF forms a scaffold-like structure that slowly releases growth factors over time.
This sustained release may provide prolonged biological signaling that supports tissue repair.
Potential benefits of PRF include:
• Gradual growth factor release
• Structural support for healing tissue
• Enhanced cellular migration
• Support for collagen and bone matrix formation
PRF is being studied in both orthopedic and dental bone regeneration procedures.
Potential Applications of Regenerative Therapies in Fracture Care
Regenerative treatments may be explored in cases where healing is delayed or when additional biological support may be beneficial.
Areas of investigation include:
• Stress fractures
• Delayed-union fractures
• Non-union fractures
• Bone defects
• Surgical bone repair support
• Joint reconstruction procedures
These therapies are typically used as adjunctive treatments alongside conventional orthopedic care, not as replacements for necessary surgical stabilization or fracture management.
Frequently Asked Questions
How long does a bone fracture take to heal?
Healing time varies depending on the bone involved, the severity of the fracture, and individual health factors. Minor fractures may heal within 6–8 weeks, while more complex fractures may take several months.
What is a non-union fracture?
A non-union occurs when a fracture fails to heal properly after several months. This can happen when there is insufficient blood supply, movement at the fracture site, or underlying medical conditions.
Are regenerative therapies a replacement for surgery?
No. In cases where surgical stabilization is necessary, regenerative therapies are typically considered supportive treatments rather than replacements for standard orthopedic care.
Are PRP and PRF derived from my own blood?
Yes. Both PRP and PRF are produced using a small sample of the patient’s blood that is processed to concentrate platelets and healing factors.
Are stem cell therapies widely used for fractures?
Stem cell therapies are being actively researched in orthopedic medicine. Their potential role in supporting bone repair continues to be studied in clinical trials and regenerative medicine research.

