Overview
Shoulder and rotator cuff injuries are among the most common musculoskeletal conditions, affecting athletes, active individuals, and aging populations alike. The shoulder is the most mobile joint in the body, but this mobility comes at the expense of stability, making it particularly vulnerable to injury, degeneration, and chronic pain.
The rotator cuff is a group of four muscles and tendons—supraspinatus, infraspinatus, teres minor, and subscapularis—that stabilize the shoulder joint and enable lifting and rotational movements of the arm. Injury to any component of this system can result in pain, weakness, limited range of motion, and functional impairment.
Common Types of Shoulder & Rotator Cuff Injuries
- Rotator cuff tendinopathy and tendinosis
- Partial-thickness and full-thickness rotator cuff tears
- Shoulder impingement syndrome
- Labral tears (SLAP lesions)
- Biceps tendon pathology
- Adhesive capsulitis (frozen shoulder)
- Degenerative osteoarthritis of the glenohumeral joint
Anatomy & Biomechanics
The shoulder complex consists of four joints working in coordination:
- Glenohumeral joint
- Acromioclavicular (AC) joint
- Sternoclavicular joint
- Scapulothoracic articulation
Rotator cuff tendons experience poor blood supply, particularly near their insertion on the humeral head, which significantly limits healing capacity and predisposes these tissues to degeneration over time.
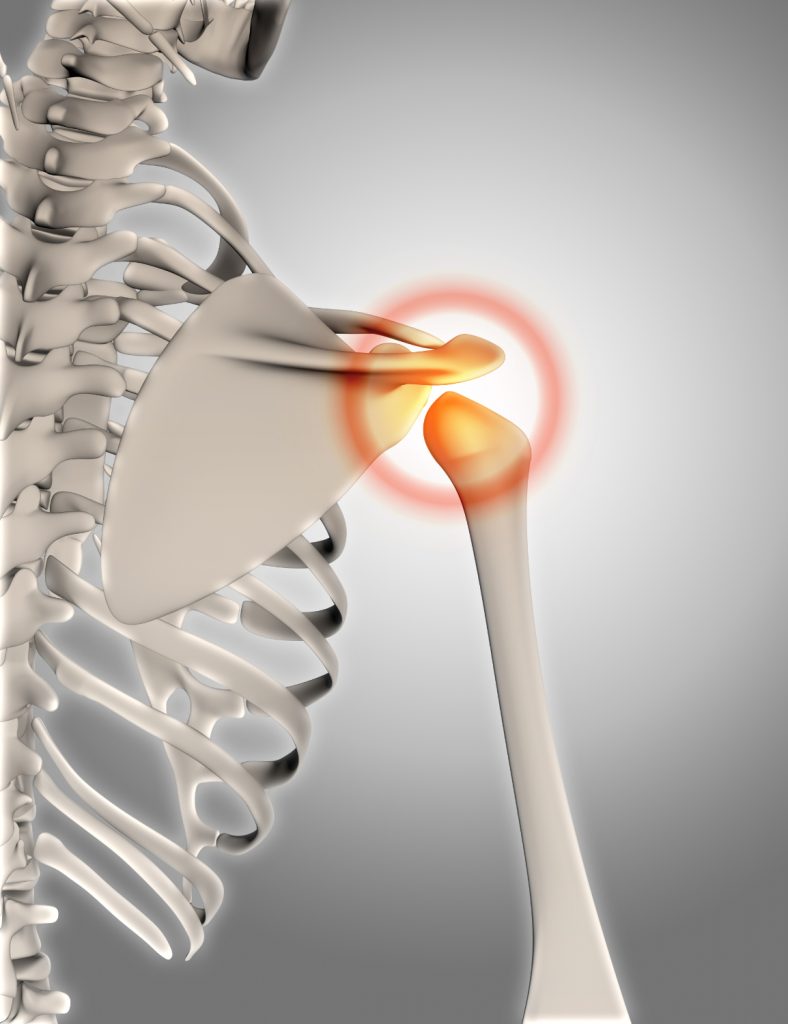
Pathophysiology of Rotator Cuff Injury
Degenerative Tendon Changes
Most rotator cuff injuries are degenerative rather than purely traumatic. Over time, repetitive microtrauma leads to:
- Collagen fiber disorganization
- Decreased tenocyte activity
- Reduced vascularity
- Accumulation of inflammatory mediators
This process, known as tendinosis, weakens the tendon structure and increases susceptibility to tearing.
Inflammatory Cascade
Injury triggers chronic low-grade inflammation characterized by:
- Elevated cytokines (IL-1β, TNF-α)
- Increased matrix metalloproteinase (MMP) activity
- Progressive extracellular matrix breakdown
Conventional Treatment Limitations
Standard treatments include:
- Rest and activity modification
- NSAIDs and corticosteroid injections
- Physical therapy
- Surgical repair in severe cases
While these approaches may reduce pain, they often do not restore tendon biology or reverse degenerative changes. Corticosteroids, in particular, may weaken tendon tissue with repeated use.
Regenerative Medicine & Biologic Therapies
Regenerative approaches aim to restore tendon health at the cellular and molecular level rather than simply suppress symptoms.
Platelet-Rich Plasma (PRP)
PRP is one of the most studied regenerative therapies for rotator cuff pathology. Mechanisms of action include:
- Delivery of growth factors (PDGF, TGF-β, IGF-1, VEGF)
- Stimulation of tenocyte proliferation
- Enhanced collagen synthesis and tendon remodeling
- Reduction of inflammatory cytokines
PRP may be particularly beneficial for partial tears, tendinosis, and post-surgical healing.
Platelet-Rich Fibrin (PRF)
PRF provides a fibrin scaffold that allows sustained growth factor release over time. Potential benefits include:
- Structural support for tendon healing
- Long-term modulation of inflammation
- Enhanced tissue integration and repair
PRF is often used when prolonged biologic signaling is desired.
Stem Cell Therapy (Investigational)
Stem cells are being explored for their ability to influence tendon regeneration through paracrine signaling.
Proposed mechanisms include:
- Promotion of tenocyte differentiation
- Modulation of inflammatory pathways
- Enhancement of angiogenesis
- Support of extracellular matrix regeneration
Stem cell therapy may be considered in chronic, refractory cases where conservative treatment has failed.
Exosome Therapy
Exosomes act as biologic messengers capable of influencing tendon healing. In shoulder injuries, exosomes may:
- Reduce chronic inflammation
- Improve mitochondrial function within tendon cells
- Enhance collagen organization
- Accelerate tissue repair signaling
Clinical Goals of Regenerative Support
- Pain reduction
- Improved shoulder strength and stability
- Restoration of functional range of motion
- Delay or avoidance of surgical intervention
Optimization of post-surgical healing when surgery is required